Why we are doing this research?
The overarching goal of the SALTY project is to add quality of life to late life for older adults living in long term care (LTC).Late life is a time when older adults and their caregivers (family/ friends) are faced with health and social issues that can impact their well-being. While living well in one’s final years is arguably a universal aspiration, it remains a challenge, particularly for those who live in LTC.
The Continuum of Late Life in Residential Long Term Care:
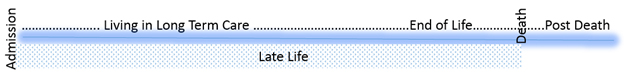
Prompted by this challenge, a team of researchers, clinicians, knowledge users, family and friend caregivers and staff from across Canada came together to develop a research project to better understand how to add quality to years in the last phase of life for people in LTC settings. This multi-disciplinary, multi-sectoral team converged on the urgent need to challenge current thinking and practice around our highly medicalized LTC system. To address this the team developed a research proposal to examine how the system can incorporate a more social relation-centred perspective and to fill knowledge gaps in how to add quality to the last phase of life for older adults in LTC settings.
What is This Research About?
SALTY’s four research aims are to:
1. Develop practical and effective approaches to longitudinal monitoring of quality of care during end of life for older adults in long term care.
2. Identify promising social and clinical approaches in late life/end of life long term care care, and understand their influence on care relationships.
3. Evaluate the implementation of a Quality Improvement (QI) project in Island Health, BC designed to improve palliative approach to end of life care in long term care facilities.
4. Examine the breadth of policies within project jurisdictions, that enable or inhibit promising approaches to care in late life long term care.
Each aim is addressed in the form of a project research stream, with a set of specific objectives. In recognition of the existence of disparities in health and social care within the long term care system, study designs will incorporate the following three lenses, where feasible: 1) dementia, 2) gender, and 3) underrepresented voices.
Monitoring care practices (Stream 1): Co-led by Dr. Carole Estabrooks and Dr. Matthias Hoben (University of Alberta). The purpose of Stream 1 is to develop a set of quality measures to monitor the trajectory of modifiable symptom burden and potentially inappropriate care practices at the end of life in late life residential care. The goal is to identify a small set of 3-4 measures each for symptom burden and potentially inappropriate care practices by using expert opinion to guide selection from a fixed set of measures in the RAI-MDS 2.0 data across Western Canada. These measures will ultimately inform our understanding of the end of life experience in residential care, as well as facilitate the implementation and evaluation of interventions to improve this experience.
Mapping care relationships (Stream 2): Co-led by Dr. Tamara Daly (York University), Dr. Ivy Bourgeault (University of Ottawa) and Dr. Katie Aubrecht (Mount Saint Vincent University). Stream 2 will involve an examination of approaches in late life/end of life residential care that considers facility-based cases that focus on care relationships. It uses relevant published and grey research and clinical data collected as part of Streams 1, 3 and 4, to identify promising social approaches in late life residential care. Promising approaches are understood as approaches that promote comfort, enjoyment and social engagement. Primary research involving qualitative research methods (interviews, focus groups, observations and cases) will allow the Team to analyze how approaches influence care relationships.
Evaluating innovative practice (Stream 3): Co-led by Dr. Kelli Stajduhar, Dr. Denise Cloutier (University of Victoria) and Dr. Leah MacDonald (Island Health, BC). Stream 3 will evaluate the Vancouver Island Implementation Project for Improving End-of-Life Outcomes in Residential Care. This project is being implemented in four sites in British Columbia. The overall goal of the Improving End-of- Life Outcomes in Residential Care project is to implement a promising palliative approach in the context of care provided in long term care facilities. The evaluation will provide evidence to support application of this project in other provinces.
Examining policy context (Stream 4): Co-led by Dr. Deanne Taylor and Heather Cook (Interior Health, BC) and Dr. Janice Keefe (Mount Saint Vincent University). Stream 4 will consider the breadth of the regulatory environment within the different jurisdictions, focusing on key areas such as safety, environmental design and educational standards that are identified by key informants. Four policy lenses will be used to ascertain ways in which policies support or limit: 1) family/friend caregiver involvement in care, centred on resident quality of life, 2) volunteer contributions to informal care for persons at late life, 3) resident preferences for comfort, autonomy and security and 4) staff flexibility to provide quality care within the regulatory environment. Following the initial assessment of regulatory complexities within and across policy domains, Stream 4 findings will be linked to ascertain the ways in which regulatory environments may impact on or provide context for other Streams’ research findings.